
Learning Objectives
By the end of this section, you will be able to do the following:
- Name the fluid component of blood and the three major types of formed elements, and identify their relative proportions in a blood sample
- Identify various blood cell types in a blood smear
- Describe and draw an erythrocyte and all five types of leukocytes
Components of Blood
Blood can be divided into a liquid component and a cellular component, each with distinct roles in transport and defense.
The two main components of blood are:
- Plasma
- Formed elements
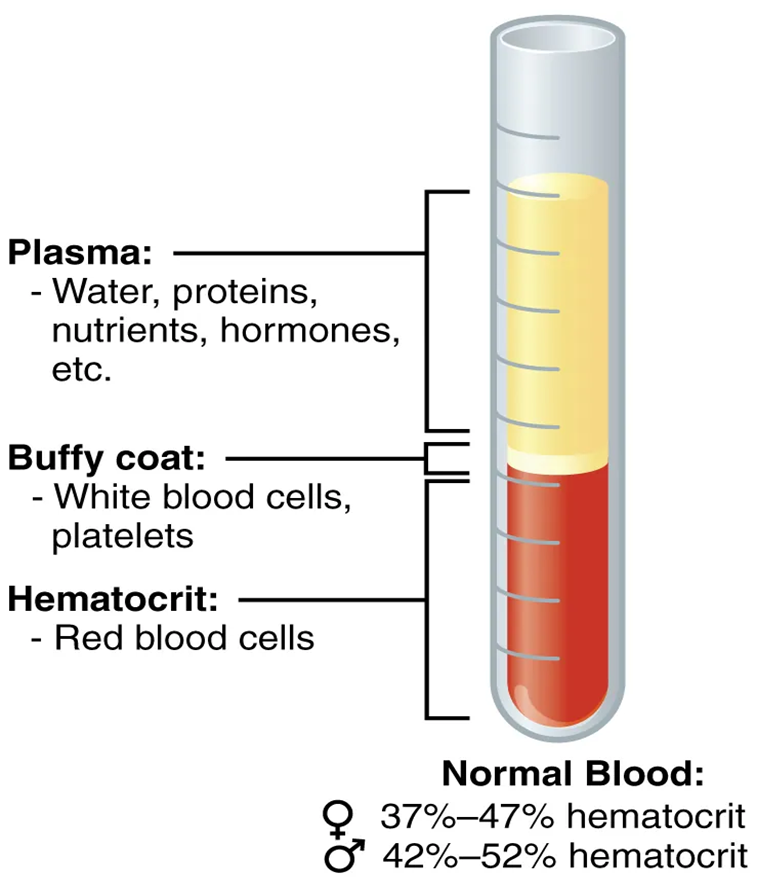
Figure 2. Composition of Blood. Centrifugation separates whole blood into plasma, a buffy coat of leukocytes and platelets, and erythrocytes. Hematocrit represents the proportion of red blood cells. Source: OpenStax, Anatomy and Physiology 2e, Figure 18.2, CC BY 4.0.
Plasma
Plasma is the liquid portion of blood in which the formed elements are suspended, making up about 55% of total blood volume. A sample of blood spun in a centrifuge reveals that plasma is the lightest component (Figure 1). It floats at the top of the tube separated from the heaviest elements, the erythrocytes, by a buffy coat of leukocytes and platelets. It is mostly water but also contains proteins, nutrients, hormones, and dissolved gases.
Plasma acts as the transport medium for many substances moving throughout the body.
Practice words
An erythrocyte is a red blood cell (RBC) that transports oxygen from the lungs to body tissues and carries carbon dioxide back to the lungs for removal. It contains the protein hemoglobin, which binds oxygen, and has a distinctive biconcave disc shape that increases surface area for gas exchange. Mature erythrocytes lack a nucleus, allowing more space for hemoglobin and making them highly efficient at oxygen transport.
A leukocyte is a white blood cell (WBC) that plays a key role in the body’s immune system by helping defend against infections, foreign substances, and abnormal cells. Unlike erythrocytes, leukocytes have a nucleus and can move out of blood vessels into tissues to fight pathogens. There are several types of leukocytes—such as neutrophils, lymphocytes, monocytes, eosinophils, and basophils—each with specialized functions in immune defense.
Formed Elements
All formed elements of the blood arise from multipotent hematopoietic stem cells in the bone marrow. Figure 2 provides a schematic overview of the formed elements of human blood, which are suspended and bathed in plasma, the liquid portion of blood. The formed elements make up about 45% of blood volume and include:
- Red blood cells (erythrocytes)
- White blood cells (leukocytes)
- Platelets (thrombocytes)
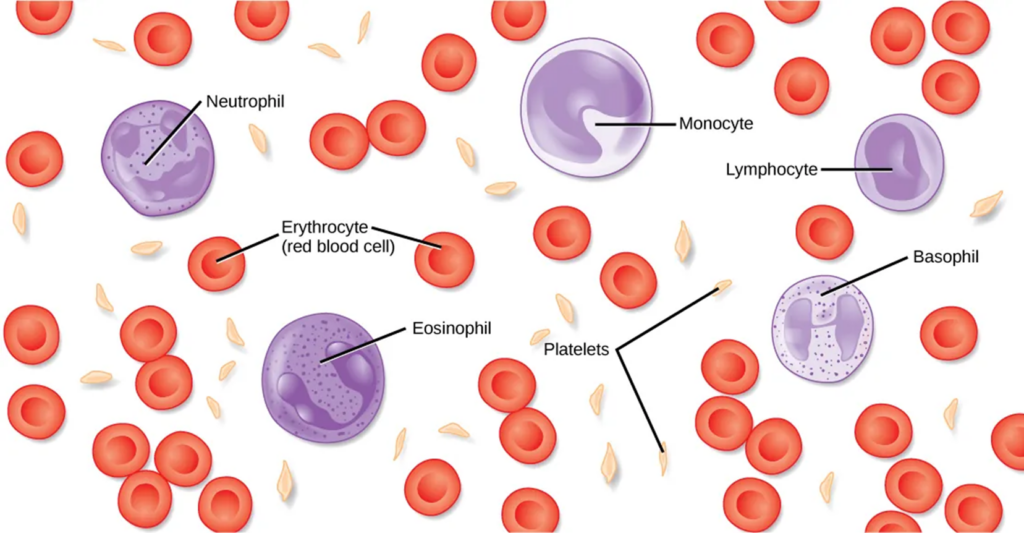
Before exploring each formed element in detail below, take a moment to examine Figure 2 closely.
What differences do you notice among red blood cells, white blood cells, and platelets? Consider their relative size, shape, abundance, and overall appearance.
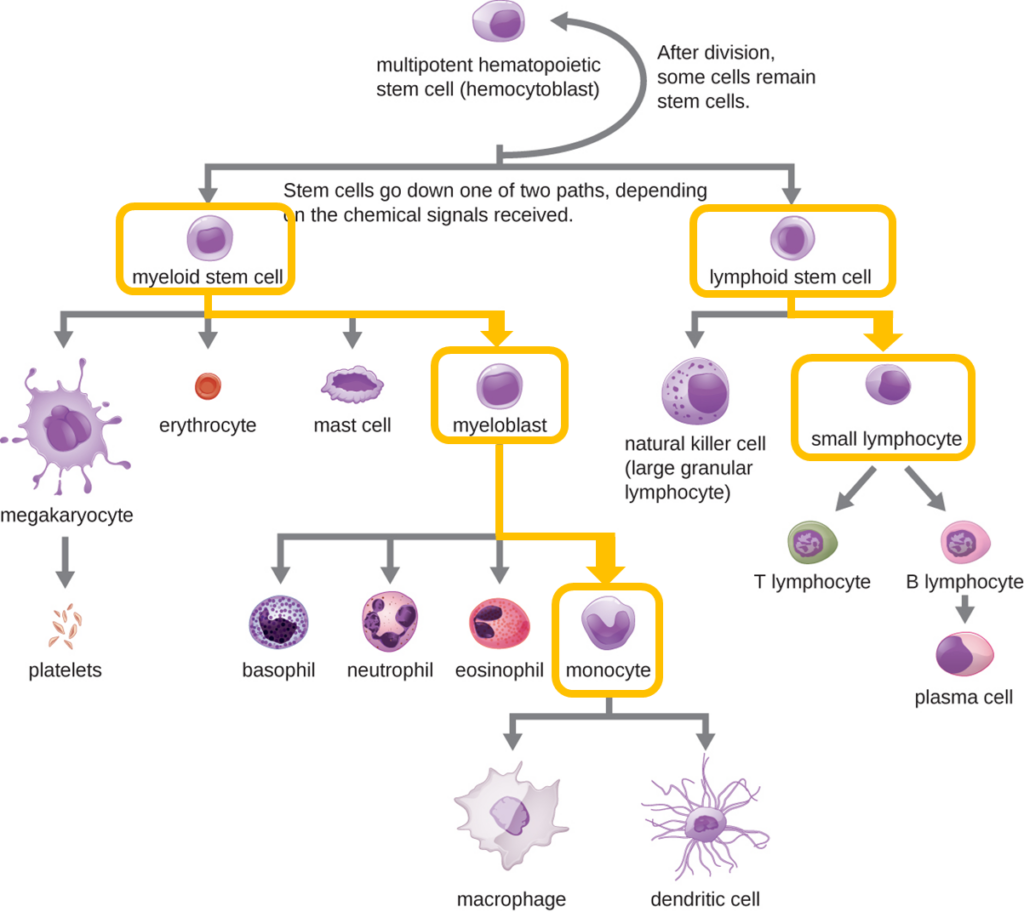
All of the formed elements of blood are derived from pluripotent hematopoietic stem cells (HSCs) in the bone marrow. As the HSCs make copies of themselves in the bone marrow, individual cells receive different cues from the body that control how they develop and mature. As a result, the HSCs differentiate into different types of blood cells that, once mature, circulate in peripheral blood. This process of differentiation, called hematopoiesis, is shown in more detail in Figure 4.
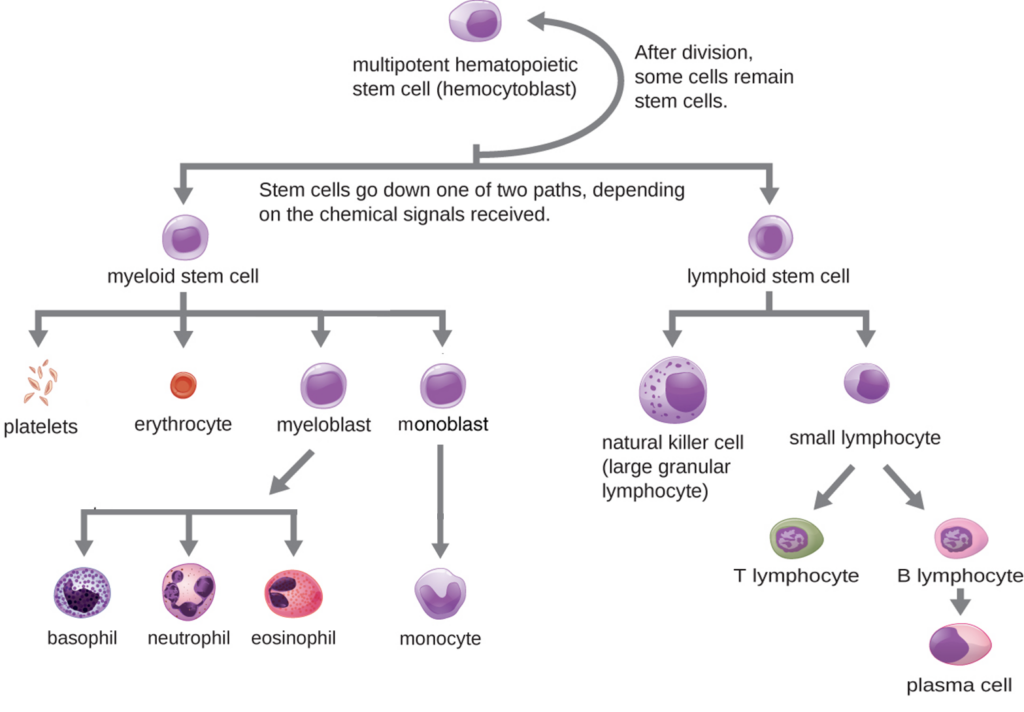
Figure 4. Hematopoietic differentiation of blood cells.
All formed elements of the blood arise from multipotent hematopoietic stem cells in the bone marrow. In this simplified diagram, differentiation is shown along two primary pathways—myeloid and lymphoid stem cell lineages. The myeloid lineage gives rise to erythrocytes, platelets, and leukocytes, including granulocytes (neutrophils, eosinophils, basophils) and the agranular monocyte. The lymphoid lineage gives rise to agranulocytes, including natural killer cells and lymphocytes (T lymphocytes and B lymphocytes, which can differentiate into plasma cells). Modified from: OpenStax, Microbiology, “Cellular Defenses.” Biology LibreTexts. CC BY 4.0.
Erythrocytes
The erythrocyte, commonly known as a red blood cell (or RBC), is by far the most common formed element. A single drop of blood contains millions of erythrocytes and just thousands of leukocytes. Specifically, males have about 5.4 million erythrocytes per microliter (µL) of blood, and females have approximately 4.8 million per µL. In fact, erythrocytes are estimated to make up about 25 percent of the total cells in the body (OpenStax, 2019).
Red blood cells are responsible for transporting oxygen throughout the body. They contain the protein hemoglobin, which binds oxygen in the lungs and releases it to tissues. Erythrocytes are biconcave disks; that is, they are thick at their periphery and very thin in the center (Figure 3). Because they lack a nucleus and most organelles, more intracellular space is available for hemoglobin molecules that transport respiratory gases (OpenStax, 2019). Red blood cells give blood its red color.
Practice your vocabulary!
A thrombocyte, also known as a platelet, is a small fragment of a cell found in the blood that is essential for blood clotting (hemostasis). Thrombocytes are formed from large cells in the bone marrow called megakaryocytes and do not have a nucleus. When a blood vessel is damaged, they quickly gather at the site, stick together, and release chemicals that help form a clot to stop bleeding.
Pluripotent hematopoietic (stem cell) refers to an early blood-forming stem cell found mainly in the bone marrow that can differentiate into all types of blood cells. These cells give rise to both major lineages: the myeloid lineage (which produces erythrocytes, platelets, neutrophils, eosinophils, basophils, and monocytes) and the lymphoid lineage (which produces B and T lymphocytes). They are essential for maintaining continuous blood cell production throughout life.Hematopoiesis is the process of forming all blood cells in the body. It primarily occurs in the red bone marrow, where pluripotent hematopoietic stem cells divide and differentiate into the different blood cell types: erythrocytes (red blood cells), leukocytes (white blood cells), and thrombocytes (platelets). This process is tightly regulated by hormones such as erythropoietin (EPO) to maintain proper blood cell levels and overall homeostasis.
The erythrocyte, commonly known as a red blood cell (or RBC), is by far the most common formed element. A single drop of blood contains millions of erythrocytes and just thousands of leukocytes. Specifically, males have about 5.4 million erythrocytes per microliter (µL) of blood, and females have approximately 4.8 million per µL. In fact, erythrocytes are estimated to make up about 25 percent of the total cells in the body (OpenStax, 2019).
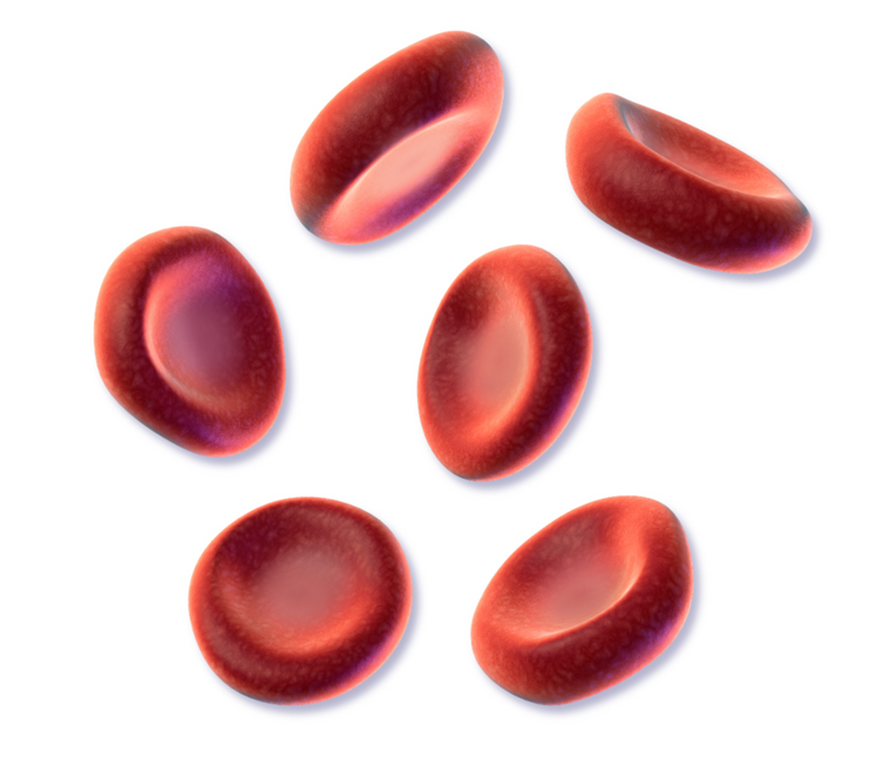
Red blood cells are responsible for transporting oxygen throughout the body. They contain the protein hemoglobin, which binds oxygen in the lungs and releases it to tissues. Erythrocytes are biconcave disks; that is, they are thick at their periphery and very thin in the center (Figure 5). Because they lack a nucleus and most organelles, more intracellular space is available for hemoglobin molecules that transport respiratory gases (OpenStax, 2019). Red blood cells give blood its red color.
White Blood Cells (WBCs)
White blood cells are part of the immune system and help protect the body against infections and foreign substances.
The five major types of leukocytes found in peripheral blood are as follows:
- Neutrophils
- Lymphocytes
- Monocytes
- Eosinophils
- Basophils
Click here to practice pronouncing and spelling each leukocyte name.
Observing White Blood Cells in a Blood Smear
A blood smear, peripheral blood smear or blood film is a thin layer of blood smeared on a glass microscope slide and then stained in such a way as to allow the various blood cells to be examined microscopically. Blood smears are examined in the investigation of hematological (blood) disorders and are routinely employed to look for blood parasites, such as those of malaria and filariasis . Cells in blood smears are commonly examined using a Wright or Giemsa stain. This staining causes cell nuclei to appear purple, while cytoplasm typically appears pink or pale blue, making differences in nuclear shape and cytoplasmic features easier to observe.
Initial Observation Activity
Figure 4 shows the major types of leukocytes observed in a stained peripheral blood smear.
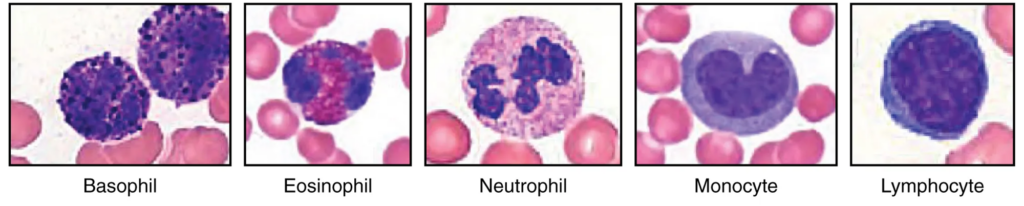
Leukocyte Observation Table (Initial Observations)
Instructions
Download Table 1 and use Figure 4 to complete it by recording all visible differences between the leukocytes.
Focus on what you actually see, such as relative cell size, nuclear shape, cytoplasmic appearance, colour, or texture. Use your own words rather than technical terms.
Table 1. Initial observations of leukocyte morphology.
| Leukocyte type | Cell size (relative to RBCs) | Nucleus shape | Cytoplasm appearance | Notable visible features |
|---|---|---|---|---|
| Neutrophil | ||||
| Lymphocyte | ||||
| Monocyte | ||||
| Eosinophil | ||||
| Basophil |
Refining Identification: Who’s Who?
Click the dropdown below to revisit and refine your observations, correcting or adding details as needed.
Who’s who?
White blood cells can be classified as granular or agranular based on the presence or absence of visible cytoplasmic granules. When identifying leukocytes on a blood smear, focus on overall cell size, nuclear shape, and the appearance of the cytoplasm.
Revised table including drawings
Download Table 2 before you review the descriptions of granular and agranular leukocytes. Fill in any new or revised information and draw each type of leukocyte.
Granular Leukocytes
Granular leukocytes include neutrophils, eosinophils, and basophils, listed from most common to least common. All are derived from myeloid stem cells and are produced in the red bone marrow. Once released into the circulation, granular leukocytes have a short lifespan, typically lasting hours to days. These cells usually possess a lobed nucleus and are classified based on the staining properties of their cytoplasmic granules, which are highlighted by specific dyes (Figure 5).
Agranular Leukocytes
There are two major types of agranulocytes:
- lymphocytes
- monocytes
Explore the figure.
These cells lack large, visible cytoplasmic granules when stained with standard dyes. Agranular leukocytes arise from hematopoietic stem cells in the red bone marrow, but they diverge into different lineages: lymphocytes develop from the lymphoid lineage, while monocytes develop from the myeloid lineage.
Agranular leukocytes typically have a round or kidney‑shaped nucleus and a longer lifespan than granular leukocytes, ranging from days to years, depending on cell type and function (Figure 6).
Lymphocytes can look like monocytes, except that lymphocytes do not have a kidney-bean shaped nucleus, and lymphocytes are usually smaller. Most of the lymphocytes are small; a bit bigger than red blood cells, at about 6-9 µm in diameter. Monocytes are the largest type of white blood cells, and can be up to 20µm in diameter. They have a large eccentrically placed nucleus, which is kidney bean shaped.
Try to identify a lymphocyte and a neutrophil in the peripheral blood smear shown below.
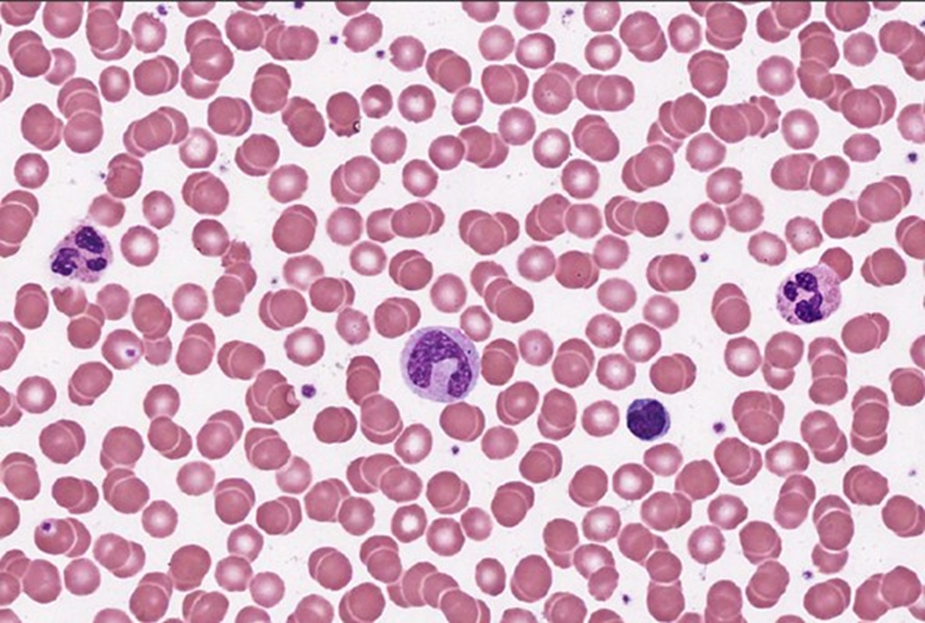
Practice your white blood cell identification skills.
Platelets
Platelets are cell fragments that play an essential role in blood clotting. When a blood vessel is damaged, platelets help form a clot that prevents excessive bleeding.
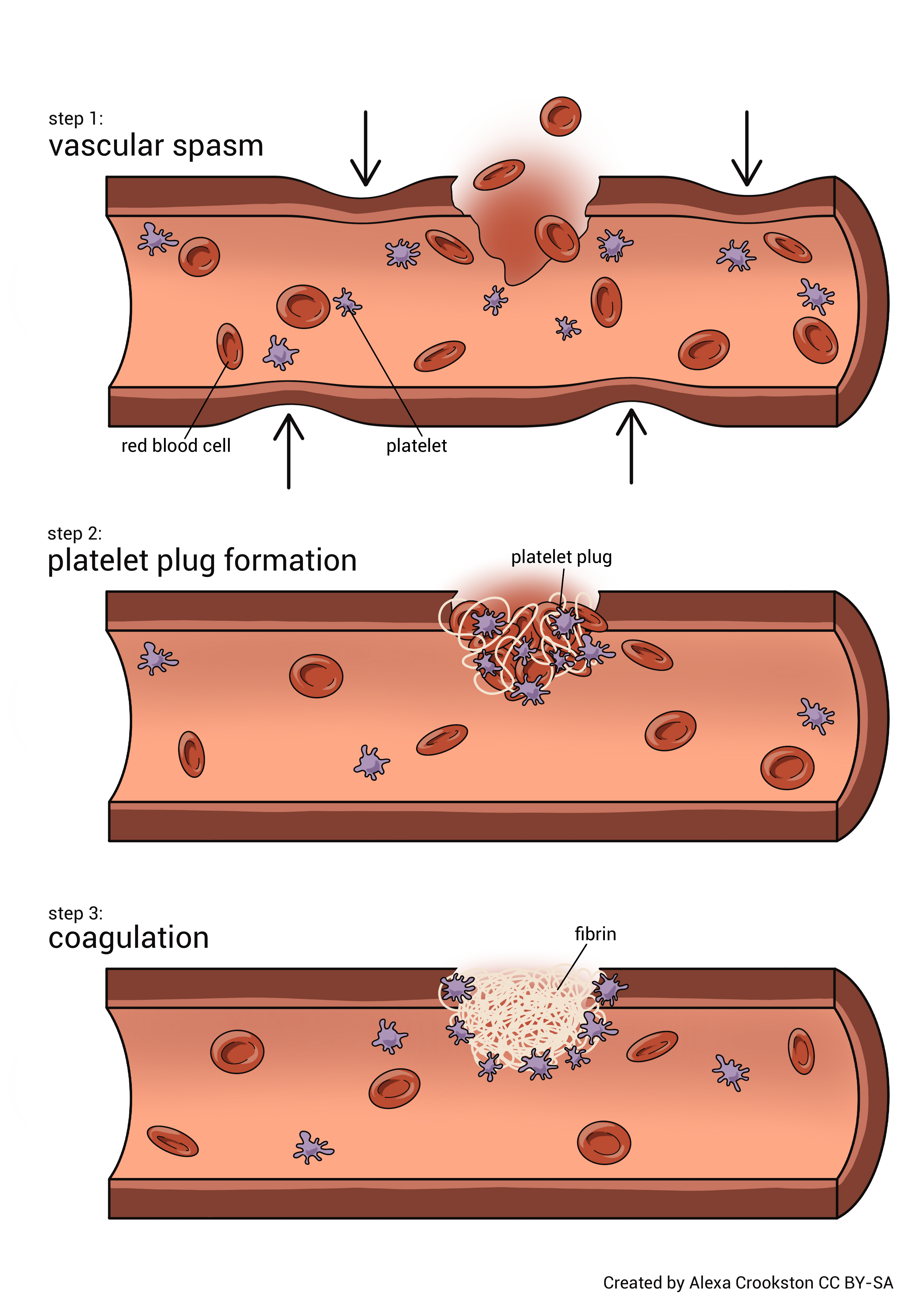
Practice Activity
Spelling Practice
References
Bliss D. 2002. Red blood cells illustration [illustration]. National Cancer Institute (US). Available from: https://commons.wikimedia.org/wiki/File:Red_blood_cells_illustration.jpg
OpenStax, Anatomy and Physiology 2e, Section 18.4, “Leukocytes and Platelets.” Illustration by OpenStax.
https://openstax.org/details/books/anatomy-and-physiology-2e. Licensed under CC BY 4.0.
OpenStax, Microbiology. “Cellular Defenses.” Biology LibreTexts. CC BY 4.0.
https://bio.libretexts.org/Courses/Sacramento_City_College/BIOL_440%3A_General_Microbiology_(Hughes)/13%3A_Week_13/21%3A_Innate_Nonspecific_Host_Defenses_(Part_B)/21.01%3A_Cellular_Defenses
Blood smear. (n.d.). Wikipedia. Retrieved April 22, 2026, from https://en.wikipedia.org/wiki/Blood_smear