Leukemia
Leukemia is a type of blood cancer that affects the cells in the bone marrow, where blood cells are produced. In leukemia, the body produces large numbers of abnormal white blood cells (leukocytes) that do not function properly.
These abnormal cells crowd the bone marrow and bloodstream, which interferes with the production of healthy blood cells such as red blood cells and platelets. This can lead to symptoms such as fatigue, infections, and easy bruising or bleeding.
There are several types of leukemia, including Acute Lymphocytic Leukemia (ALL) and Chronic Myelogenous Leukemia (CML).
Acute Lymphocytic Leukemia (ALL)
Acute Lymphocytic Leukemia (ALL) is a rapidly progressing cancer that affects lymphocytes, a type of white blood cell involved in the immune response.
In ALL, immature lymphocytes multiply quickly in the bone marrow and bloodstream. Because these cells are not fully developed, they cannot properly fight infections.
ALL is the most common type of leukemia in children, although it can also occur in adults. With modern treatments such as chemotherapy, survival rates for many patients with ALL have improved significantly.
Figure 1 – ”Myeloid Neoplasms and acute leukemia” Maslak P. 2016. Lymphoblasts – 1. Hematologyorg. [accessed 2026 Apr 1]. https://imagebank.hematology.org/image/2397/lymphoblasts–1.
Chronic Myelogenous Leukemia (CML)
Chronic Myelogenous Leukemia (CML) is a slower-developing leukemia that affects myeloid cells, which are precursor cells that normally develop into several types of blood cells including granulocytes.
CML is associated with a specific genetic abnormality known as the Philadelphia chromosome, which forms when parts of two chromosomes swap places. This mutation causes uncontrolled cell growth in the bone marrow.
Unlike ALL, CML often progresses slowly and may not cause symptoms in its early stages. Many patients are diagnosed during routine blood tests.

Figure 2 – Blood Test Comparison Normal Leukemia Blood Stock Vector (Royalty Free) 2358432531 | Shutterstock. 2023. Shutterstock. [accessed 2026 Apr 1]. https://www.shutterstock.com/image-vector/blood-test-comparison-normal-leukemia-cancer-2358432531?trackingId=951d1048-4279-4ce5-9aab-1e759c38c5af&listId=searchResults.
Sickle Cell Disease
Sickle cell disease (SCD) is a genetic blood disorder that affects the protein hemoglobin found inside red blood cells. Hemoglobin carries oxygen from the lungs to the rest of the body.
In people with sickle cell disease, a mutation in the beta-globin gene changes the structure of hemoglobin. This causes hemoglobin proteins to stick together and form long chains, which distort red blood cells into a crescent or “sickle” shape.
Unlike normal red blood cells, which are flexible and round, sickled cells are:
- Rigid
- Sticky
- More fragile
Because of their shape, sickled cells can block small blood vessels. This can reduce oxygen delivery to tissues and cause severe pain episodes called sickle cell crises.
Other complications may include:
- Chronic anemia
- Organ damage
- Increased risk of infection
- Reduced life expectancy without treatment

Figure 3 – Sickle Cell Disease Diagram Comparison Blood Stock Vector (Royalty Free) 2579187539 | Shutterstock. 2025. Shutterstock. https://www.shutterstock.com/image-vector/sickle-cell-disease-diagram-comparison-blood-2579187539.
Sickle Cell Trait
Not everyone who inherits the sickle cell gene develops the disease.
Individuals who inherit one sickle cell allele and one normal allele have sickle cell trait. These individuals usually do not experience symptoms because most of their hemoglobin is normal.
However, they can pass the sickle cell gene to their children.
Malaria and Sickle Cell: An Evolutionary Connection
One of the most well-known examples of natural selection in humans involves the relationship between sickle cell trait and malaria.
Malaria is a life-threatening disease caused by parasites transmitted through the bites of infected mosquitoes.
In regions where malaria is common, particularly sub-Saharan Africa, people with sickle cell trait have a survival advantage. Their red blood cells make it more difficult for the malaria parasite to reproduce.
Because individuals with sickle cell trait are more resistant to severe malaria, the sickle cell gene has remained common in populations from malaria-endemic regions.
This phenomenon is known as balanced polymorphism, where a genetic trait persists in a population because it provides a survival advantage under certain environmental conditions.
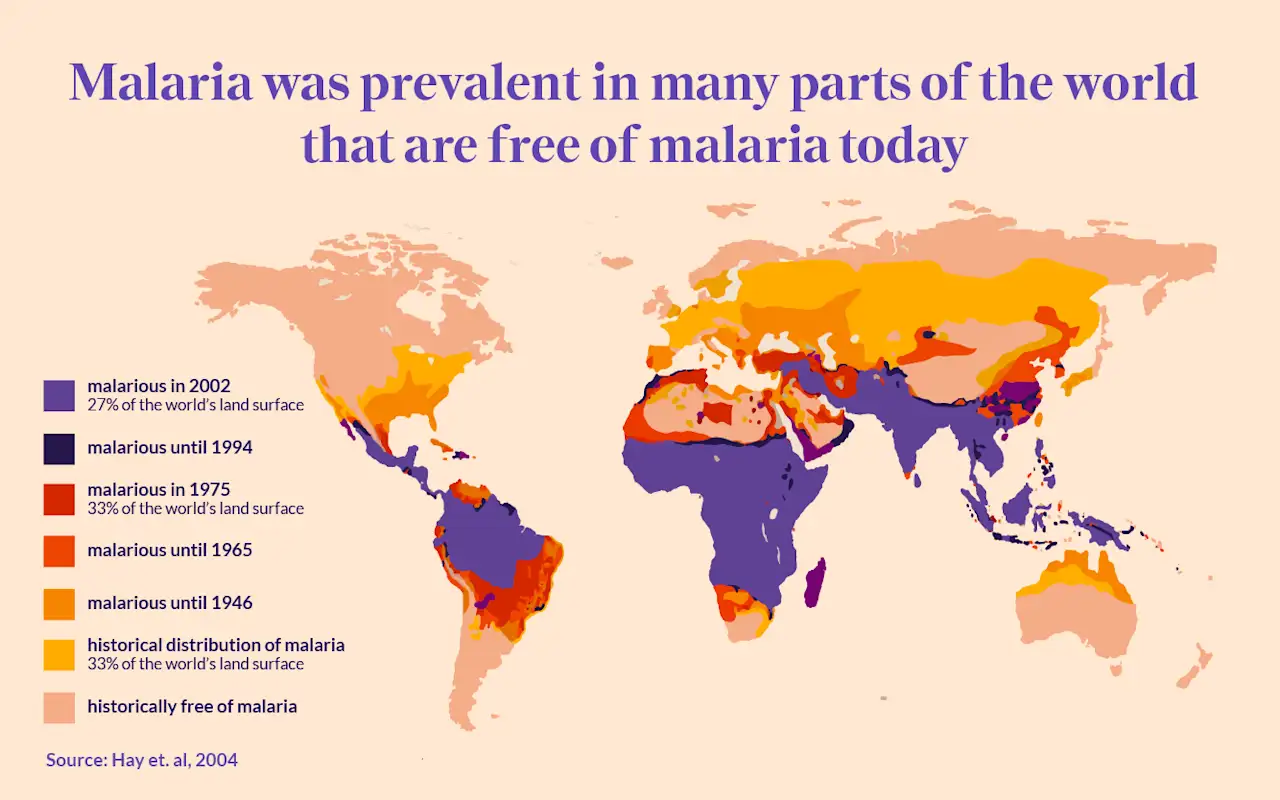
Figure 4 – Teh D. 2021 Oct 21. Sickle cell anemia: How our red blood cells evolved to fight malaria. HealthMatch. https://healthmatch.io/blog/sickle-cell-anemia-how-our-red-blood-cells-evolved-to-fight-malaria.
Did You Know?
People with sickle cell trait often have increased protection against severe malaria, which is why the sickle cell gene is more common in regions where malaria has historically been widespread.
This is one of the most widely cited examples of natural selection in human populations.
Equity, Diversity, and Inclusion (EDI) in Sickle Cell Disease
Sickle cell disease is an important example of how genetics, ancestry, healthcare access, and systemic inequities intersect in medicine.
- Ancestry and Misconceptions:
Sickle cell disease is most commonly associated with individuals whose ancestors come from:
- Sub-Saharan Africa
- The Mediterranean
- The Middle East
- India
- Parts of South and Central America
However, it is important to understand that sickle cell disease is not tied to race, but rather to geographic regions where malaria historically occurred.
This distinction highlights the difference between biological ancestry and socially constructed ideas of race.
- Historical Bias in Research and Funding
Despite being one of the most common inherited blood disorders in the world, sickle cell disease has historically received less research funding and medical attention compared to other genetic diseases.
For example, diseases that primarily affect populations of European ancestry, such as cystic fibrosis, have historically received significantly more funding per patient in biomedical research.
These disparities reflect broader patterns of systemic inequities in healthcare research and funding.
- Barriers in Healthcare
Many individuals living with sickle cell disease face challenges within healthcare systems, including:
- Delayed diagnosis
- Limited access to specialized treatment
- Under-treatment of pain
- Healthcare bias and stigma
Patients experiencing sickle cell crises often require urgent pain management, but research has shown that some patients report not being taken seriously when seeking care.
Addressing these issues requires improving:
- Medical education
- Cultural competency in healthcare
- Access to specialized care
- Representation and Awareness
Increasing awareness of sickle cell disease is an important step toward improving patient outcomes.
Public health initiatives now focus on:
- Newborn screening programs
- Genetic counseling
- Community education
- Research into new treatments, including gene therapy
These efforts help promote health equity and ensure that patients with sickle cell disease receive appropriate care and support.